
10 Formalising a precise and workable definition for CLI has been problematic. There are a number of definitions and classifications of PAD available to define the presence and severity of disease 5, 18, 19 but they are not used consistently in clinical practice. 15- 17 Critical limb ischaemia How do you define CLI? 14 Survival in patients with CLI is poor, with one-year mortality rates being over 30% and approximately 25% of patients undergo major amputation within one year. The prevalence of CLI has been reported as 0.24% in an unselected population of 40–69 year olds, with diabetes increasing the risk. 1 The term ‘critical limb ischaemia’ (CLI) is reserved for the most advanced form of PAD where limb viability is becoming threatened. The overall incidence of amputations (minor or major) is significantly higher in those with diabetes (2. PAD can result in increased morbidity and impair quality of life through intermittent claudication, rest pain, lower limb ulceration, 13 or amputation.

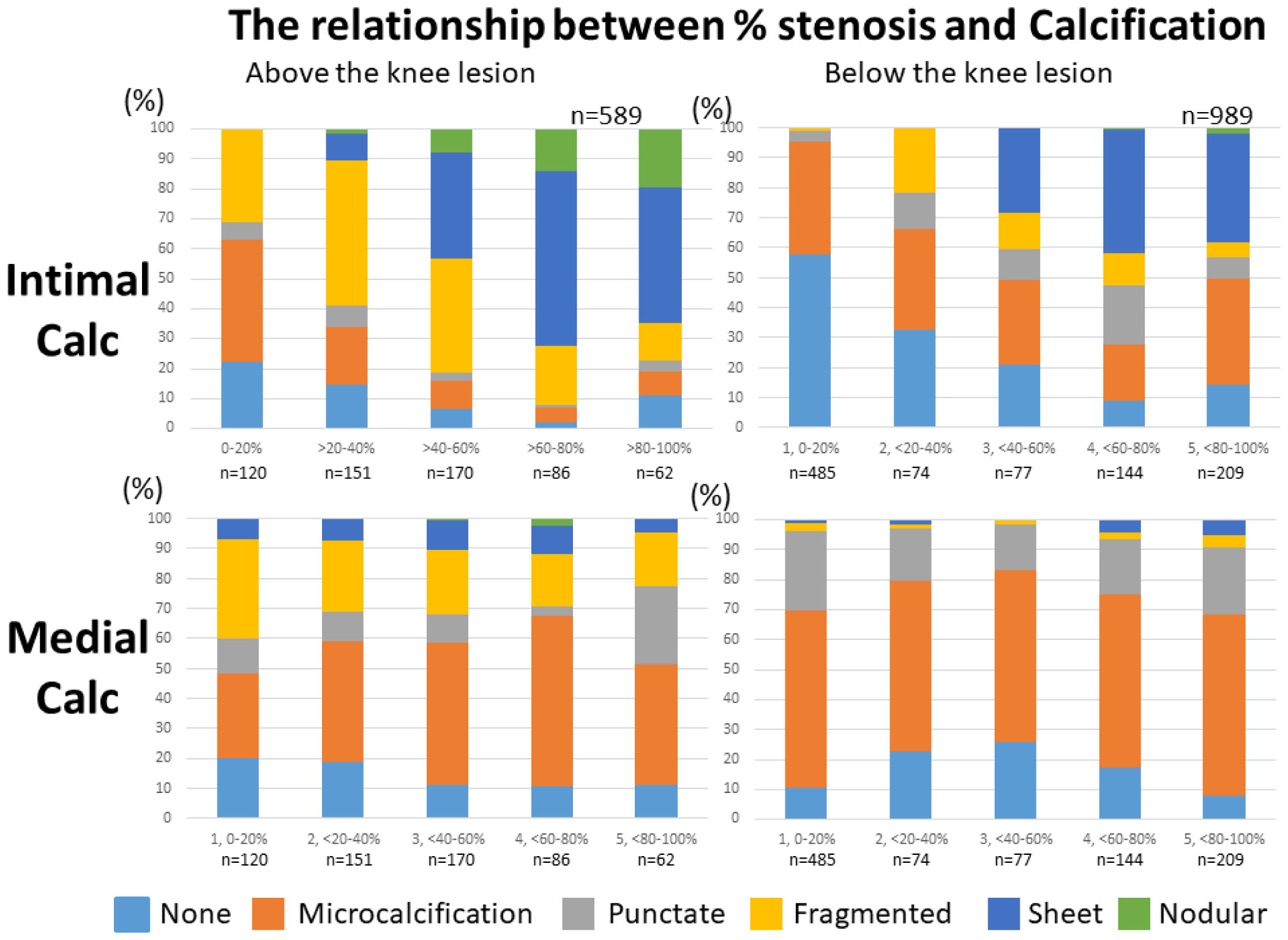
12 This propensity for more distal disease influences the types of endovascular and surgical treatment required to revascularise a compromised limb. In diabetes patients with PAD there is a greater tendency for the below knee (‘tibial’ or ‘crural’) vessels to be diseased than in the non-diabetic population. 11 All patients with PAD should therefore have their diabetes and hypertension well controlled, receive appropriate statin and antiplatelet therapy unless contraindicated, and smoking should be discouraged. Increasing HbA 1c is associated with an increasing risk of PAD.
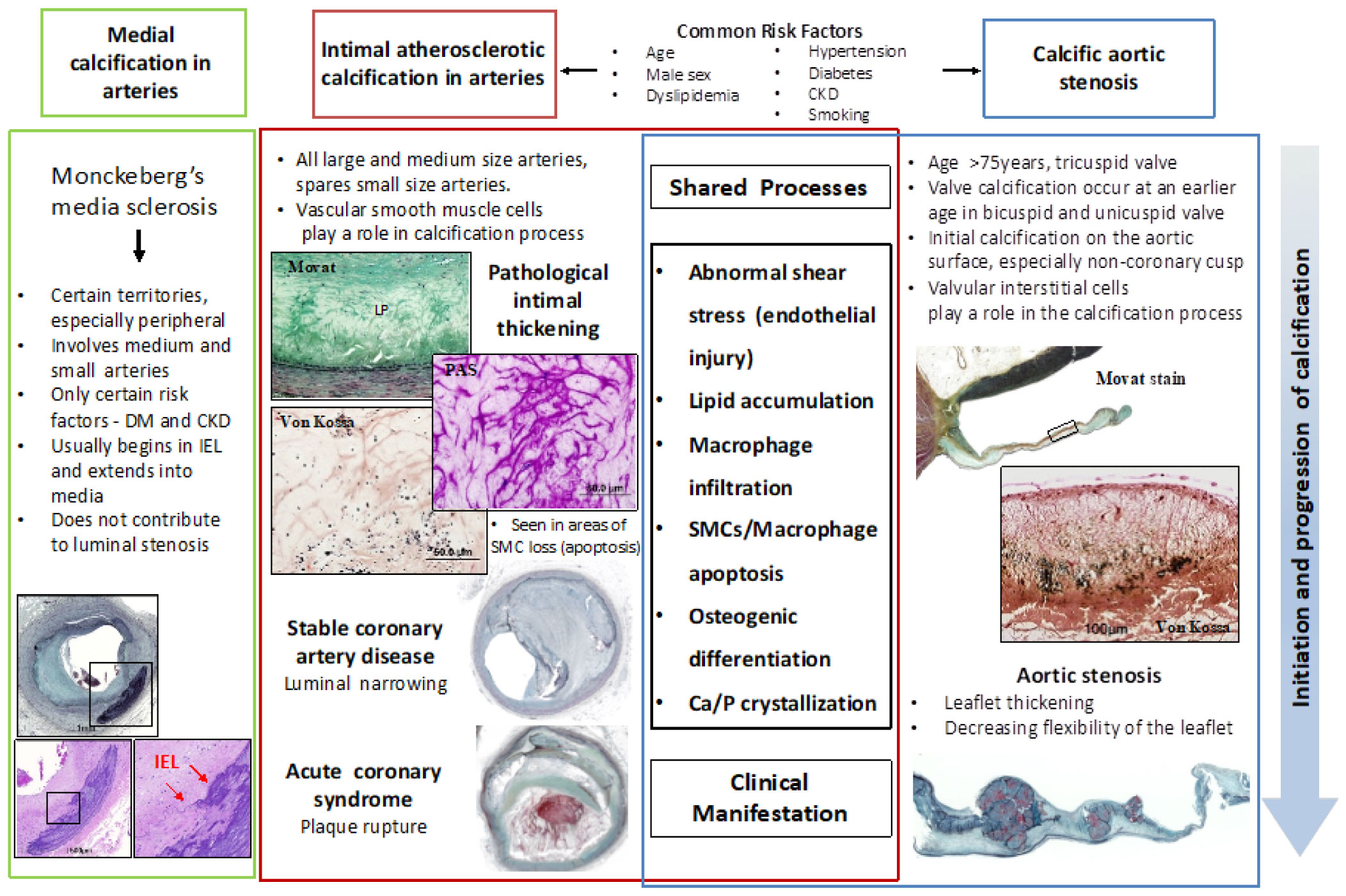
8- 10 The pathological processes of atherosclerosis in those with and without diabetes are broadly similar, as are the main risk factors which include smoking, diabetes, increasing age, abnormal lipid profile, hypertension, and renal disease. PAD (whether symptomatic or not) should be recognised as a strong surrogate marker for cardiovascular and cerebrovascular disease. 6 In Scotland, data have shown that the annual incidence of PAD development is 5. 6 In those with diabetes the risk of PAD is increased 2–4-fold. Peripheral arterial disease (PAD) affects 3–10% of the general population overall, rising to over 15% in those aged over 70 years, 5 with cigarette smoking and diabetes being the two most common potentially modifiable risk factors in its development. Peripheral arterial disease How common is it?
However, the article will not cover the specific management of intermittent claudication, or the acutely ischaemic limb. This review will concentrate on the detection, 3, 4 subsequent investigation and specialist management of critical limb ischaemia (CLI). Despite foot disease being costly to the individual, with half of all amputations in England occurring in people with diabetes, 1 and to the NHS in financial terms, 2 it remains a relatively neglected complication. Foot disease is one of the most common complications in patients with diabetes, with peripheral arterial disease (PAD) being a major factor in the pathogenesis of both foot ulceration and amputation.
